|
|
|
Malignant Melanoma - Information for Medical Professionals
Definition and Description
Malignant melanoma is a malignant skin tumor arising most often from epidermal melanocytes and rarely from dermal melanocytes. Its incidence is increasing, this tumor being the most frequent cause of death due to a skin disease. Malignant melanoma can be divided into four main clinical subsets due to a combination of clinical and pathological features:
- superficial spreading melanoma
- nodular melanoma
- lentigo maligna melanoma
- acral lentiginous melanoma
Approximately 70 per cent of melanomas appear on clinically normal skin, whereas 30 per cent occur in pre-existing nevi.
Incidence and Epidemiology
Malignant melanoma occurs among all adequately studied racial and ethnic groups. The frequency of its occurrence is closely associated with the constitutive colour of the skin, and depends on the geographical zone. Incidence among dark skinned ethnic groups is 1 per 100,000 per year or less, but among light-skinned Caucasians up to 50 and higher in some areas of the world. The highest incidence rates have been reported from Queensland, Australia with 56 new cases per year per 100,000 for men and 43 for women. The current estimated annual incidence of melanoma in the United States among whites, adjusted for the same standard population and for the same year (1987) is 14 and 11. In Northern Europe the incidence is than 5 per 100,000 in countries of low insolation. Cutaneous malignant melanoma is the most rapidly increasing cancer in whites. The annual increase in incidence rates has been estimated to be between 3 and 7%, mortality rates increasing less quickly, though.. These estimates suggest a doubling of rates every 10-20 years. The cumulative lifetime risk for melanoma is now in the order of 1 : 25 in Australia and it has been estimated to be around 1 : 75 in the United States by the year 2000. 1 out of every 105 American born in 1993 will develop malignant melanoma in his or her lifetime. In contrast, the risk in 1935 was only 1 in 1,500, in 1960 1 in 500, and in 1980 1 in 250. Malignant melanoma is now the forth most common cancer in Australia and New Zealand, the seventh most common in the USA and Canada, the tenth most common in Scandinavia and eighteenth most common in the United Kingdom. In contrast, for Africans and Asians the annual incidence rate of malignant melanoma is only 0.2 to 0.4 per 100.000 population, affecting mainly the palms, soles, and mucous membranes.
Figures from the U.S. suggest a statistically significant increase in thin tumours (<1mm) in all age groups except in men under 40 years of age. Thick tumours (>or=4mm) increased statistically significantly only in American males aged 60 years or older.
The male : female ratio is 1 : 1 in the U.S. and Australia. In Europe, the sex incidence shows a slight female preponderance in most countries. The sex ratio for incidence of melanoma varies with incidence: it is higher in females than in males in areas of low insolation and low incidence rates.
In contrast to NMSC, which mainly affects older individuals, the frequency of melanoma peaks in young people aged 20-45 years, although age-specific rates continue to rise with age. Approximately 50% of melanomas occur in individuals under 55 years of age. It is very rare prior to puberty, and when it does occur in children, about 50% of cases arise in giant congenital nevi.
Although we talk in general terms about the epidemiology of melanoma, this tumour has been subdivided on the basis of histological and clinical classification into different tumours. Some of these subtypes have different characteristics epidemiologically, both in incidence and mortality rates and also in factors likely to causation (e.g. sunlight exposure). (Marks 2000).
Etiology and Pathogenesis
The following environmental, phenotypic and genetic factors interact in the etiology of malignant melanoma. The tumor is in large part due to intermittent burning sun exposure of fair skin, though.
Environmental factors
- Sun exposure: The highest incidence of melanoma has been reported from areas with long hours of sunlight throughout most of the year. Studies reported lower risks for melanoma among people who resided in a low ultraviolet environment in childhood compared with those who resided in a high UV environment. The sun exposure-related risk seems to be greatest for intense intermittent exposure of non-sun-acclimatized skin rather than continual exposure. Exposure in childhood appears to be particularly important, as sunburns in childhood will be remembered many years later. Recreational activity leading to sunburns in adulthood, such as sailing has also been incriminated as an etiological factor.
- Artificial UV sources: Several case-control studies of melanoma risk and tanning lamp use have demonstrated a positive relation, suggesting that longer wave artificial UVA may play a part in the etiology of melanoma in addition to exposure natural sunlight. Association of melanoma with PUVA (combination of psoralen (P) and longwave ultraviolet radiation (UVA)) therapy has also been reported. This topic is still controversial, though, and further studies are needed.
- Socioeconomic status: Several studies have reported that melanoma is more prevalent in those of high socioeconomic status. An explanation of this finding may be the fact that the latter can better afford holidays in areas of high UV intensity, as well as expensive outdoor hobbies like sailing, which increase the risk of melanoma due to intermittent intense sun exposure.
Phenotypic factors
- Fair skin, freckles, red hair: These phenotypic characteristics increase the risk of melanoma.
- Number of melanocytic nevi: The total number of melanocytic nevi, dysplastic or banal, has been reported by several groups as a strong risk factor.
Genetic factors
Familial melanoma: Between 2 and 5% of melanoma patients have a positive family history of melanoma in at least one first-degree relative. In approximately 30% of melanoma patients abnormalities on chromosome 9p21 are seen. Several melanoma-susceptibility genes are discussed, one of them being p16.
Xeroderma pigmentosum: In this genetically determined disorder, defective DNA repair mechanisms lead to excessive chronic UV damage and subsequent development of different sun-related skin tumors, including melanoma, in sun-exposed areas.
Melanoma evolves from benign melanocytes forming nevi or, more likely, from fields of progressive hyperplasia followed by dysplasia on clinically normal skin or mucosa. Early melanoma tends to grow within the epidermis, displaying a radial growth. This slow unrestricted phase of growth does not show any metastatic potential. With progression, tumor growth extends vertically into the underlying dermis (vertical growth), where melanoma cells form expansive nests and nodules, and metastases can develop through invasion of tumor cells into dermal lymphatic and vascular channels. Melanoma may show different growth patterns, the monophasic growth pattern consisting of rapid vertical growth only. The biphasic growth pattern is characterized by a slow radial growth phase of months to years followed by a relatively rapid vertical growth phase.
Diagnosis
Four steps may be taken in the diagnosis of malignant melanoma.
1. Patient history
Changes in size, shape or height of a lesion, as well as changes in color, itching, crusting, or bleeding of a tumor might point to a malignant melanoma. A personal and family history of atypical nevi and malignant melanoma should also be assessed.
2. Naked-eye inspection
Several clinical features may be common to all the clinical subsets of melanoma, including the following criteria which aid clinical diagnosis of melanoma (ABCDE-rule):
Several clinical features may be common to all the clinical subsets of melanoma, including
the following criteria which aid clinical diagnosis of melanoma (ABCDE-rule):
- Asymmetry
In which one half does not match the other half
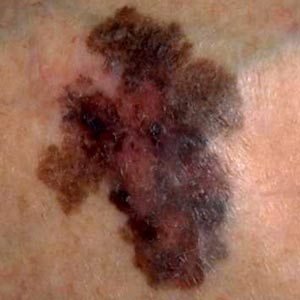
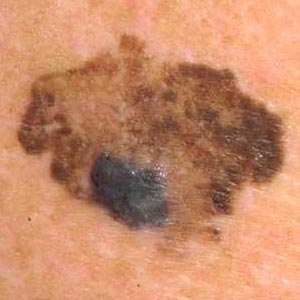
- Border irregularity
with blurred, notched, or ragged edges
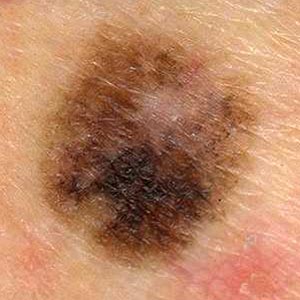
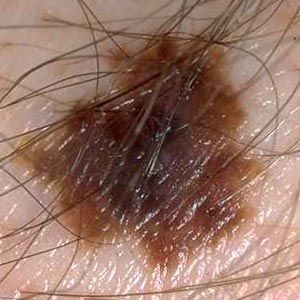
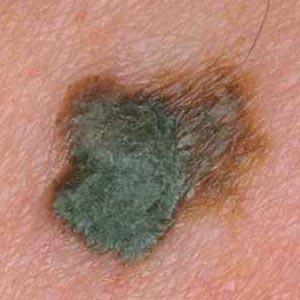
- Color irregularity
pigmentation is not uniform. Brown, black, tan, red, white, and blue can all appear in a melanoma.
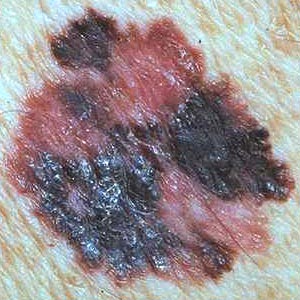
- Diameter
greater than 6 mm (the size of a pencil eraser). Growth in itself is also a sign.
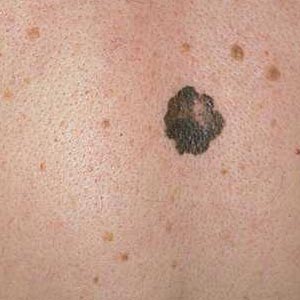
- Elevation
a raised surface can also be a sign
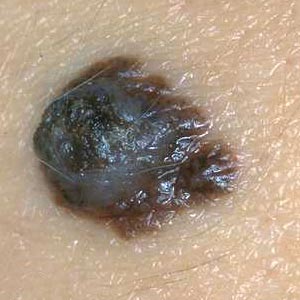
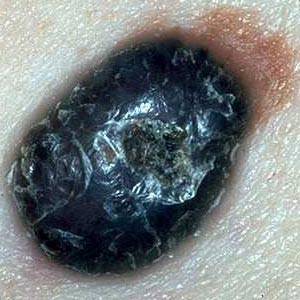
3. Dermatoscopy
Dermatoscopy (also called epiluminescence microscopy) allows for a detailed surface analysis of a skin lesion by using a hand-held device emitting light which passes the epidermal skin layer. Prior to examination, immersion oil should be placed onto the lesion surface. This procedure makes the superficial epidermal layer transparent and allows for inspection of the deeper zone of the epidermo-dermal junction.
With dermatoscopy, both sensitivity and specifity of diagnosis may be improved. However, the benefits of this method depend on training and experience with its use.
The following findings may point to a malignant melanoma when the lesion is examined with a dermatoscope:
- irregular dark pigment network
- uniform black or bluish pigmentation with only remnants of a pigment net
- areas of pigment confluence at the edge
- radial streaming
- pigmentary pseudopods
- a whitish, blue or milky veil in presence of a network
- bluegray areas or white scarlike areas
4. Biopsy
If after transversing the previous steps the diagnosis is still unclear, the correct procedure in the case of a lesion 1 - 2 cm in diameter or less is an excision biopsy with a narrow surrounding margin of approximately 2 mm normal skin.Incisional biopsies present the possibility that malignant cells may be dislodged into blood vessels at the time of the procedure and are therefore not recommended.
If the clinical appearance strongly suggests a thin melanoma, an excision biopsy may be unnecessary. In this case a one-stage definitive excision with a 1-cm margin around the lesion both laterally and in depth is a common procedure.
Symptoms, Signs, and Course
According to the clinical findings, several types of melanoma are distinguished, which have differing appearances and may take a somewhat different course.
Superficial spreading melanoma (SSM).
This is the commonest type of melanoma on white skin, comprising over 70% of cases. It occurs most frequently in middle-aged patients. In an early stage, when it is still in the horizontal growth phase,it presents as an irregularly shaped brown or blackish macular lesion. After progressing to the vertical growth phase, the lesion will become palpable. Color variation in SSM is often pronounced, with a mixture of brown, black, grey and red shades. Partial regression may cause central pigment loss, resulting in whitish areas. In an advanced growth stage, bleeding and ulceration may occur.
Nodular melanoma (NM).
This type of melanoma affects most commonly individuals in the fifth or sixth decade. The lesion presents as an elevated, dome-shaped blue-black or reddish brown nodule. Ulceration and bleeding occur frequently. The tumor is characterized by an, if present at all, only short phase of horizontal growth and rapid vertical growth.
Lentigo maligna melanoma (LMM).
This type of melanoma develops from lentigo maligna, a precancerous lesion characterized by prolonged lateral extension (much longer period of horizontal growth than in SSM). Most lesions occur on the face in older individuals. Lentigo maligna is a flat, brown or black lesion, which grows very slowly. In time, a raised central nodule will present, indicating a transition to the vertical growth phase and the development of lentigo maligna melanoma.
Acrolentiginous melanoma (ALM).
Melanoma developing on the palms and soles,, as well as on toes and fingers, represents only 10% of cases in Whites, but over 50% of all melanomas on Black and Asian skin. The tumor is characterized by a macular, lentiginous pigmented area around a nodule. Mechanical stress may lead to erosion and ulceration. Subungual melanomas present as pigmentations of the nail bed, and are commonly diagnosed at a late stage in development.
Amelanotic melanoma.
This type of tumor presents as an erythematous or pink, sometimes eroded, nodule. Amelanotic melanoma is often confused for other tumors, and sometimes only the histological examination provides the right diagnosis.
Mucosal melanoma.
This rare type of melanoma is seen in the oral cavity, on the genital mucosa or in the perianal area. It first presents with extensive, irregular macular pigmentation. Mucosal melanoma is often diagnosed at a late stage, when already deeply penetrating tumors have formed.
Prevention and Prophylaxis
According to the risk factors for malignant melanoma, the following preventive measures are recommended:
- UV exposure should be minimized. Prolonged sunbathing, especially of non-sun-acclimatized skin, as well as the use of tanning lamps is not advisable. Children under three years of age should be kept in the shades.
- Sun protection should be achieved through adequate clothing. Broad-brimmed hats, shirts with long sleeves and sunglasses are recommended. Children should be especially carefully dressed when playing outside.
- The use of adequate sunscreens is recommended. This should not lead to prolonged sunbathing, though, thinking that all risks have been ruled out with the use of sunscreens.
- Sunburns should be avoided, especially in children.
- Present nevi should be checked. Patients with pre-existing nevi should be trained to check on them at regular intervals, especially looking for changes in size, color and shape. Patients should also be taught to attentively watch new spots on their skin regarding to rapidity of growth and change in color. When changes are noticed, this should lead immediately to visiting a dermatologist.
- Individuals with multiple nevi and/ or dysplastic nevi should be checked regularly by a dermatologist. Suspect nevi should be removed.
Differential Diagnosis
Nodular Melanoma:
Superficial Spreading Melanoma:
Lentigo Maligna Melanoma
Acrolentiginous Melanoma:
Amelanotic Melanoma:
Complications
Malignant melanoma may ulcerate, and superinfection is possible. Metastasis may occur at an early stage. Usually melanoma metastasizes at first over the lymphatic system into the surrounding skin or into the regional lymph nodes. Later, internal organs may be affected, particularly the lungs, liver, brain and the heart, as well as the bones, through blood-borne metastasis. Cutaneous metastases may also develop because of bloodstream metastasis.
Treatment
Different factors play a role in the management of melanoma, including the tumor's extent, the advancement of the disease, the patient's age and general health and many other. The treatment of malignant melanoma therefore must be chosen individually. The following enumeration lists different stages of melanoma with possible therapeutic procedures.
Primary tumor treatment
As far as possible, all melanomas should be surgically removed with a resection margin depending on the tumor thickness.
- Tumor thickness < 1mm: A horizontal and vertical resection margin of 1 cm is recommended.
- Tumor thickness > or = 1 mm: The resection margin should comprise 2 - 3 cm, depending on the anatomic conditions.
The patients should also be considered for sentinel node biopsy. (This procedure involves injecting blue dye or a radiolabelled colloid into the skin at the site of the melanoma, opening the skin surgically over the relevant draining lymph-node basin, and biopsying the node into which the dye or radiolabelled colloid first drains.)If the sentinel node is free of tumor, it is unlikely that there will be tumor cells in other nodes. If the node is positive, a full lymph-node dissection is recommended.
- Tumor thickness > 1,5 mm: Some centers recommend an adjuvant therapy with alpha- interferon (e.g. Roferon A). During the treatment phase, alpha-interferon 2A is applied daily subcutaneously for 3 weeks in a dose of 3 million I.U. During the following 49 weeks, the substance is applied only three times a week in the same dosage.
If surgical treatment of primary melanoma is not possible, radiotherapy is recommended.
Treatment of in-transit-metastases
Cutaneous in-transit-metastases should be surgically removed as far as possible. If this procedure is not an option, the following therapeutical measures should be considered:
- If the metastases are localized on an extremity, an intraarterial hyperthermal cytostatic drug perfusion as well as a regional lymph-node dissection are possible therapeutical strategies.
- If hyperthermal drug perfusion is not an option, radiotherapy is a possible treatment.
- Other possibilities include a combination of local sensitization with DNCB (production of an allergic contact dermatitis over superficial cutaneous metastases) and cytostatic dacarbazine, immune therapy with tumor vaccines, and an adjuvant therapy with alpha-interferon 2B according to the protocol of the EORTC Melanoma Cooperative Group.
Treatment of lymph node metastases
- Radical lymph-node dissection is recommended as far as possible. Postoperative radiotherapy may follow. Adjuvant interferon therapy in the context of a clinical trial may be an option after surgical removal of the metastases.
- If surgical treatment is not possible, radiotherapy alone may give good palliative results. Several melanoma vaccines are in the course of evaluation for patients with inoperable lymph node metastases.
Treatment of distant metastases
It is advisable that patients with advanced disease should be treated in specialized centers by a multidisciplinary team. Several treatment options as well as clinical trials of therapy are available depending on the affected organs, the number of metastases and the patient's general health.
Surgery
In case of an operable solitary metastasis (neuro)surgical procedures are recommended. Palliative surgery may be necessary in case of perforation, abscess formation and internal bleeding.
Radiotherapy
Radiotherapy is indicated in case of brain metastases when surgical procedures are not possible or advisable. Stereotactic radiation is applied in case of up to 2 brain metastases. When more than 2 metastases have been detected, radiation of the whole brain is a common procedure. Stereotactic radiation with a gamma-knife may be applied even in case of more than 2 brain metastases. Palliative radiotherapy is advisable in case of bone metastases.
Chemotherapy
Inoperable remote metastases without brain involvement
In this case several treatment options and clinical trials of therapy are available, including
- Dacarbazine. Studies have shown partial of complete remission in 20 - 40% of treated patients.
- Polychemotherapy combining cisplatin, dacarbazine, BCNU and tamoxifene, or Polychemoimmunotherapy with interleukin-2 and alpha-interferon added.
- Chemoimmunotherapy combining temozolomide with alpha-interferon (clinical trial)
- Currently only as second-line therapy in case of ineffective first-line chemotherapy: several tumor vaccines, chemotherapy with paclitaxel and carboplatin.
Inoperable brain metastases
- Chemotherapy with fotemustine
- Chemotherapy with temozolomide, eventually in combination with radiation
Isolated multiple liver metastases
- Intraarterial chemotherapy into the A. hepatica propria with fotemustine.
- Local hyperthermy.
After surgical removal of all metastases or successful chemotherapy a postjuvant immunotherapywith interleukin-2 and alpha-interferon may be possible in the context of a clinical trial.
This listing of possible therapeutical options does not claim to be complete. Besides established treatments, it includes experimental chemo- and immuno(chemo)therapies which are being applied in specialized centers and whose efficacy is still being investigated.
Prognosis
Several prognostic factors for malignant melanoma are being discussed, the best established factors being the tumor thickness,which has been introduced by Breslow, and the invasion levels introduced by Clark et al. The following enumeration gives an outline of relevant prognostic factors.
- Tumor thickness. The distance between the granular layer in the epidermis and the deepest invasive melanoma cell measured in millimeters represents the tumor thickness. A histological examination of a slide from the thickest area of the melanoma is necessary to determinate this figure. Melanomas less than 0,75 mm thick present only a low metastatic risk according to Breslow, whereas tumors 3mm thick or more present a very high one.
- Levels of invasion into the dermis. This histological classification is based on the melanoma's depth of penetration:
- Level 1: Tumor cells only in the epidermis
- Level 2: Tumor cells throughout the basement membrane zone and as far as the papillary dermis
- Level 3: Tumor cells as far as the boundary zone between the papillary and the reticular dermis
- Level 4: Tumor cells invade the reticular dermis
- Level 5: Tumor cells invade the subcutaneous adipose tissue
The 5-year survival rate with level 1 or 2 is over 90%, whereas with level 4 or 5 it is approximately 50 - 60%.
- Mitotic activity. The mitotic index (mitoses/mm2) varies inversely with survival.
- Ulceration. Macro- and microscopic ulceration is an additional poor prognostic sign.
- Vascular invasion. The presence of tumor cells in vessels indicates a worse prognosis.
- Localization. Melanomas on the extremities have a better prognosis than those on the head or the trunk. Melanomas in the anogenital region have a poor prognosis, as they are often discovered in late stages.
- Sex. Women statistically have a somewhat greater chance to survive than men.
|
|

|
|

|
|
